Diabetic foot & Ulcers
About Diabetic foot & Ulcers
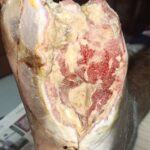
Diabetic foot
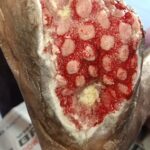
After debridement & VAC dressing
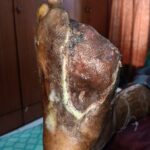
Skin grafting
Signs of Diabetic Foot Problems
- Changes in skin color.
- Changes in skin temperature.
- Swelling in the foot or ankle.
- Pain in the legs.
- Open sores on the feet that are slow to heal or are draining.
- Ingrown toenails or toenails infected with fungus.
- Corns or calluses.
- Dry cracks in the skin, especially around the heel.
- Non healing wounds over foot.
How does Diabetic foot happen?
Foot problems in diabetes can occur due to restricted blood flow and unnoticed cuts and infections that develop due to numbness in the area.
A person with diabetes needs regular podiatric checks to ensure that any foot problems do not develop into complications.
If any swelling or wound develops immediately consult a Plastic Surgeon.
Treatment
It requires a multimodality treatment. But first of all it should be understood that all diabetic foot doesn’t need amputation,if treated timely.
If any Vascular pathology is there,then help of a Vascular Surgeon is taken.
Physician/diabetologist is also needed for hyperglycemia management.
Wounds are treated by Plastic Surgery like skin grafting, flap surgery.
Rehabilitation is most important part of treating diabetic foot.Modified shoe wears are advised for diabetic foot patients.
Foot Care
- Inspect your feet daily.
- Bathe feet in lukewarm, never hot, water.
- Be gentle when bathing your feet.
- Moisturize your feet but not between your toes.
- Cut nails carefully.
- Never treat corns or calluses yourself.
- Wear clean, dry socks.
